Acute Coronary Syndrome (ACS)
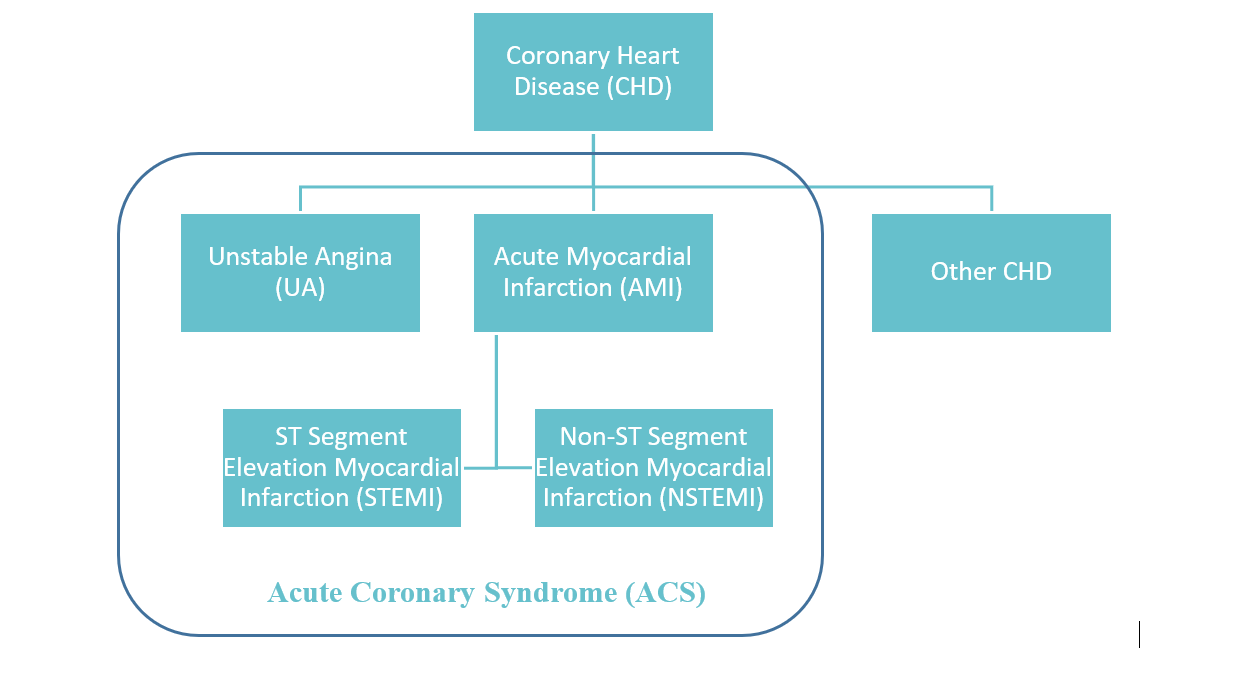
Acute coronary syndrome (ACS) includes the diagnoses of acute myocardial infarction (AMI), commonly known as heart attack and can be further differentiated into ST-elevation myocardial infarction (STEMI) and non-ST-elevation myocardial infarction (NSTEMI), and unstable angina (UA). In the USA, more than 8 million patients present to the Emergency Department each year for chest pain and suspected ACS. Of those, only about 2 million patients (20-25%) are diagnosed with ACS. The remaining chest pain patients do not have ACS and are at low risk for major morbidity and mortality. The unnecessary use of resources and long wait-times compounded with the escalating degree of emergency department crowding makes it highly beneficial to be able to shorten the time required to stratify the chest pain patients by risk for ACS and for early discharge.
Acute Coronary Syndrome (ACS) Definition
Cardiac Markers and Risk Stratification of ACS
Quantification of cardiac biomarkers Troponin I (cTnI), Myoglobin (MYO), N-terminal pro-B-type natriuretic peptide (NT-proBNP) and Creatine Kinase-muscle/brain (CK-MB), in human whole blood or plasma, either individually or in combination, had been used as an aid in the diagnosis and risk stratification of patients of chest pain suspected of ACS at the emergency department and primary care sites. To date, cardiac troponins are regarded as the best biomarkers in ACS for detecting myocardial necrosis and risk assessment due to their high sensitivity and specificity. However, troponin release is typically delayed for several hours after the onset of ischemic injury.
Testing of a panel of early and late cardiac markers has been shown to potentially reduce the frequency of serial testing and accelerate evaluation process in conjunction with other mainstay diagnostic tools for rapid diagnosis and subsequently timely treatment or early ED discharge.
Spot Profiler TA-CVD
The Spot Profiler Cardiovascular Disease (TA-CVD) test panel is capable of quantitatively detecting 6 cardiac biomarkers in a small sample of human whole blood or plasma, simultaneously, in 15 minutes: cTnI, MYO, NT-proBNP, CK-MB, D-Dimer and FABP.